
Originally developed in the 1960’s as part of the Russian space program, the science of heart rate variability has since found broad application in cardiac medicine, though in the last two decades this technology has spread into the elite levels of strength and conditioning.
Providing a glimpse into an individual’s autonomic nervous system profile, heart rate variability measurements accurately pinpoint an athlete’s location on the fatigue-recovery-supercompensation curve. Such data can provide the missing link in optimizing an athlete’s programming – especially those who require the highest levels of physical preparation.
Stress and the Autonomic Nervous System
The primary way in which the brain communicates with the periphery of the body is by sending messages down the spinal cord and out through the many branches of the nervous system. The branch of the nervous system that most are familiar with is the conscious, voluntary nervous system. This branch is used in performing a squat, kicking a ball, or striking an opponent – an athlete decides to move and it happens.
Behind the scenes, though, lies another branch of the nervous system that regulates a myriad of tasks we’d rather not spend our days worrying about. This branch projects to organs besides skeletal muscle and controls actions such as digestion, salivation, blood pressure, heart rate, and many others. Most of the communication occurring in this branch is unconscious and automatic – it is thus termed the autonomic nervous system and is highly responsive to stress.
The goal of the autonomic nervous system is to maintain homeostasis, and it does so by utilizing its two subsystems – the sympathetic nervous system and the parasympathetic nervous system.
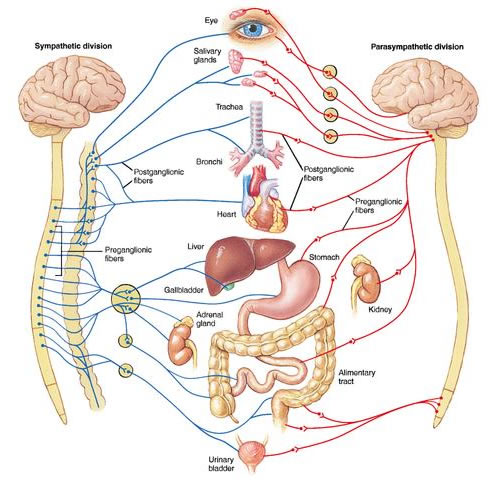
In the most basic sense, the sympathetic nervous system acts to speed up certain processes within the body. In The Wisdom of the Body, the eminent 20th century physiologist Walter Canon termed this our “fight-or-flight” response, effectively coining the phrase. The sympathetic system is responsible for raising our heart rate at the onset of a stressor, increasing blood pressure, and dumping glucose into the blood to fuel activity.
In contrast, the parasympathetic nervous system works in opposition, effectively slowing everything back down. The decrease of heart rate and storage of nutrients are two of the many “rest-and-digest” activities mediated by this system.
Homeostasis is then maintained through a physiological seesaw. For the athlete, intense training presents a large stressor to the body, invoking a strong sympathetic response to meet the increased metabolic demands. Post-workout, as the sympathetic tone subsides, the parasympathetic system becomes facilitated and drives the rest and repair necessary to get things back to normal. Ideally, these two systems remain balanced in their efforts, each ramping up and down as needed.
If a technology existed that could assess this sympathetic/parasympathetic balance, coaches could gain an excellent understanding of an athlete’s physiological state and corresponding location on the fatigue-supercompensation continuum. Information like this could drive effective, evidence-based programming decisions. For example, adjustments in volume could be made on the fly specific to the recovery status of an athlete’s physiology.
Fortunately, this technology does exist and, as mentioned above, it’s called heart rate variability (HRV).
The Science and Measurement of
Heart Rate Variability
There seems to be a misconception by some that the heart, as it beats away in the ribcage, acts like a metronome, adhering to a strict cadence at all times. In reality, the heart beats through a wide spectrum of rhythms throughout the day – these beat-to-beat variations are what the science of heart rate variability is targeting. Given that the cardiovascular system is largely controlled through the actions of the autonomic nervous system, analysis of HRV provides some great insight into these control mechanisms.
For example, when the body is battling a stressor, the variation between beats tends to be lower (i.e., less heart rate variability) and it assumes a more metronome-like quality. This situation is indicative of higher sympathetic nervous system activity – the “fight-or-flight” response is ramped up to handle the homeostatic challenge. Conversely, as the variability of the heart rate increases, the body assumes more of a rest-and-repair status, indicating increased activity of the parasympathetic nervous system.
Specific to athletes, we want strong sympathetic nervous system activity during their training to fuel the highest levels of performance, but we also want them to be able to shut that system off so they can effectively recover for subsequent session.
To use an automobile for comparison, it’s hard to slow down if you can’t take your foot off the gas. Constant activation of the sympathetic nervous system creates an unfavorable shift in the sympathovagal balance, greatly increasing the likelihood of fatigue and overtraining.
Heart rate variability is typically quantified through the use of an electrocardiogram (ECG) and measurements can take between 5 minutes and 24 hours, depending on the goals of the measurement. For athletes, 5-10 minutes seems to provide an accurate picture; for things like circadian variation, longer exposure times are necessary.
The image below provides an example of what the ECG output data might look like.
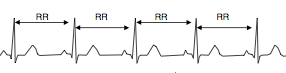
The peaks in the above wave provide a glimpse into the cardiovascular electrical activity when the ventricles are depolarized – we call this the QRS-complex. The first order of business when assessing HRV is to identify the successive QRS-complexes, so that R-R intervals (drawn above) can be determined. It’s these intervals that provide the information necessary to determine a person’s beat-to-beat variability.
Further mathematical analysis, the description of which exceeds the nature of this review, provides a frequency polygon like the one pictured below.
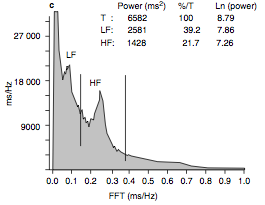
The most important thing to recognize on the above graph is the LF and the HF, standing for low frequency and high frequency, respectively. These frequency measurements are used to quantify the activity of the two branches of the autonomic nervous system.
Work by Selman et al. (1982) and Eckberg (1997) has shown parasympathetic activity largely accounts for HF, while LF is comprised of output by both the parasympathetic and the sympathetic systems. A ratio between these two measurements, called the LF/HF ration, is often used to assess the fractional distribution between the two systems and is an important marker of sympathovagal balance.
While the application of this technology has been broad across its 50-year history, the following studies highlight its efficacy when applied to monitoring applied training stresses and predicting potential physiological exhaustion.
Weightlifting Performance and HRV
In the 2011 paper entitled Parasympathetic Nervous Activity Mirrors Recovery Status in Weightlifting Performance After Training, Chen et al. set out to determine whether measurements of heart rate variability, and more specifically parasympathetic power, could be used to assess recovery status after weight training.
The study design included a collection of seven male weightlifters (19.3 ± 0.3 years). All had been training for more than 6 years prior to the study and had competed at the national or international level.
To determine the HRV modulation during the recovery period, these men were subjected to a 2-hour training session following a 10-day detraining period – their performance was then reassessed at intervals across the recovery to assess changes. HRV measurements were to be taken before training and 3, 24, 48, and 72 hours into recovery. Along with HRV, blood samples were extracted to measure serum levels of DHEA-S and creatine kinase, both markers of tissue damage and neural repair mechanisms. Lastly, subjective muscular pain scores were recorded on a 10-point scale.
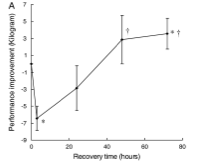
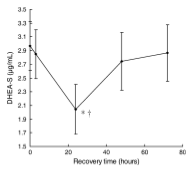
What these researchers found was a high correlation between the measured parasympathetic power and the markers of fatigue, recovery and performance. Note the similarities in the graphs below that highlight back squat performance, hormonal levels, and HF power.
 |
 |
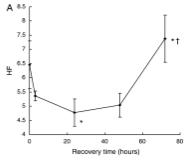 |
As the performance declined after the initial bout, we see the simultaneous suppression of both DHEA-S and HF power, which slowly return to normal over the 72-hour period. The initial decrease in DHEA-S serum levels is explained by increased consumption to fuel neural repair – this biological response is evident in many stress conditions (Gudemez et al. 2002, Lee et al. 2006).
There is strong biological plausibility for the decreased HF power, as well. As the training load of these subjects increased, the autonomic nervous system shifted to a more sympathetic dominant-state, which signified an increased demand for recovery. In 2004, Iellamo et al. showed a similar shift from parasympathetic-to-sympathetic predominance in rowers as their training volume increased. Studies like these provide strong support towards the accuracy of HRV measurements with respect to fatigue state.
If you want to learn how HRV can be used to meet both anaerobic and aerobic performance goals, I highly recommend you take the 8weeksout.com free course, The HRV Training Revolution.
Learn more about The HRV Training Revolution>
HRV in Middle-Distance Runners
A 1999 prospective cohort study by Pichot et al. assessed HRV in seven national-level French middle-distance runners, aged 24.9 ± 4.8 years, across an intense, four-week training block. The structure of the block was designed to present near-exhaustive training sessions for the first three weeks, and then deload in the fourth week.
Pichot et al. had this to say about their results:
“Our data confirm the impressive autonomic changes that occur with 3 wk of intensive physical training, consisting in a global and progressive decrease in heart rate variability and in a tendency toward a progressively lower parasympathetic and higher sympathetic drives.”
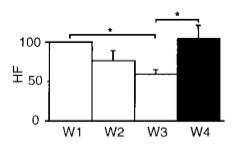
The graphs below illustrate the HF power suppression incurred by these athletes and the shift towards sympathetic dominance through the LF/HF ratio.
 |
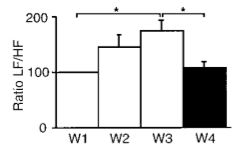 |
These results mimic those shown in a 1998 study by Uusitalo et al., which highlighted an increased resting LF/HF ratio in endurance athletes across a six-to-nine week overtraining protocol – an increase not incurred during a normal six-to-nine week block.
Many claim resting heart rate measurements to be an accurate barometer for assessing recovery, but Pichot and his colleagues make a point to explain just how unreliable resting heart rates can be in determining an athlete’s fatigue status.
Across the three intense training weeks, these runners experienced an average increase in resting heart rate of only 3.74 beats per minute – this worked out to about a 9% change across the seven subjects. Not only is a change like this rather insignificant, it’s impossible to isolate this physiological variation to a single component given its dependence on a multitude of environmental factors.
Now contrast this with the more than 40% variation in heart rate variability across the same time period. Sensitivity like this provides a much greater gauge of an athlete’s overreaching/overtraining status during a training block, especially given HRV’s consistent baseline accuracy (Hohnloser et al. 1992, Huikuri et al. 1990).
HRV and the Immune System
Modeling the relationship between stress and the immune system is one of the landmark discoveries in the field of stress physiology, first noted close to seventy years ago by the Austrian physiologist Hans Selye.
In his lab rats, Selye discovered that thymicolymphatic atrophy, or the breakdown of immune tissues, along with adrenal hypertrophy and peptic ulcers create a triad of symptoms forming some sort of nonspecific response by the body to generic unpleasantness. He would go on to term this the general adaptation syndrome, which we now just refer to as the stress-response. While some of Selye’s theories have since been disproven, the association between increasing levels of stress and immunosuppression remains well supported in the literature.
Though the pathophysiology is complex, the basic idea is that sympathetic nervous system hormones, beta-endorphins, CRH, and, most prominently, glucocorticoids all act to suppress immunity during the stress-response. For example, glucocorticoids can directly cause shrinking of the thymus gland, halt the formation of new lymphocytes, and make circulating lymphocytes less responsive to certain cytokines. They can even cause lymphocyte apoptosis through a variety of mechanisms.
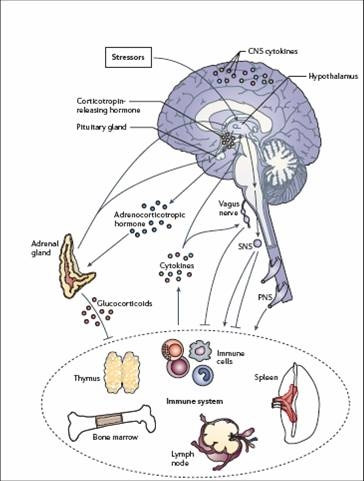
All this leads to a simple fact – the more stress the body incurs, the more likely it is to become infected.
While this should worry just about anyone reading, it’s the elite athlete or coach who should be most concerned. Creating high performance requires the application of substantial stress, which invariably pushes one’s physiology closer and closer towards pathology. In this regard, HRV provides valuable predictive data that can be useful in implementing prophylactic measures before illness manifests and performance suffers.
In a well-constructed 2011 prospective cohort study, Hellard et al. set out to examine the association between HRV and illness in 18 elite swimmers, each competing on either the national or international level.
The most impressive quality about this study’s design is its duration. The researchers measured HRV in these athletes every Monday for two full years, between 2003 and 2005. That’s over 1508 weeks of total observation across the cohort.
The main results of this study were the following:
- During the winter, the national-level swimmers were more prone to illness than the international-level swimmers.
- The weeks prior to the appearance of an upper-respiratory tract and pulmonary infection, and also soft-tissue pathology, were characterized by an increase in parasympathetic activity (more on this below).
- During the weeks in which a swimmer had an upper-respiratory tract or a pulmonary infection, a shift in the sympathovagal balance toward sympathetic predominance was noted.
- In the winter, measurements of lower parasympathetic power and higher sympathetic power were predictive of soft-tissue pathology. (Cold temperature was one of many generic stressors Selye used to produce the general adaptation syndrome in his rats.)
While most of the results should come as little surprise, the second item listed concerned me a bit. How, with so much discussion regarding the positive effects of parasympathetic power, was higher HF measurement predictive of illness? The authors of the study provide a brilliant explanation.
The period preceding the clinical expression of the illness could serve as the incubation phase for the pathology, which tends to be about five days for upper-respiratory tract and pulmonary infections. The boost in parasympathetic power is probably involved in the body’s attempt to mount an early immune response to foreign, inflammatory stimuli. Once the pathology has “won” and begins multiplying and scattering its viral and bacterial agents into the bloodstream, the body undergoes the classic immunological stress-response, characterized by an increase in sympathetic activity.
Though more research is required in this area to be sure, the researchers recommend increased medical attention and prophylactic measures be given to those athletes who experience a sudden increase in parasympathetic power followed by a shift towards sympathetic dominance.
Along with these results, Allgorve et al. (2008) showed increased exercise intensity characterized by a sympathovagal shift towards sympathetic dominance to be destructive to salivary immune cells known as immunoglobulins. Clearly, there is a link between training stress and immunological function – HRV provides an effective way to monitor the interplay between the two.
The Bottom Line on Heart Rate Variability
For the sake of brevity, I’ve only picked a handful of studies in support of HRV – there are dozens more showing similar promise towards the realm of strength and conditioning. Aside from its efficacy, heart rate variability is also much easier to measure than other fatigue assays such as serum lactate or hormonal testing. And with BioForce HRV, the technology is finally be affordable for everyone.
In the right hands, programming optimization through the science of heart rate variability can be the determinant in reaching new levels of performance.
Learn more about how HRV can take your training to the next level HERE

I recently got a HR with R-R capability, How long should I rest to get a baseline for HRV? And do I need to completely rest or could I still do low intensity skill work?
You need to be completely stable and in a stable position. I’d suggest getting 3-5 minutes of data once your heart rate has stabilized. The only way to get anything meaningful out of R-R intervals pulled from a heart rate monitor is to export it into kubios.
I’m using the iThlete until Bioforce HRV arrives. The iThlete guide insists that readings be taken while standing, but I have gotten some seemingly erratic results from this. Readings taken while seated are producing very different, and more consistent numbers. Joel, do you recommend sticking with seated readings for Bioforce HRV?
With BioForce HRV I recommend taking the measurement either laying on your back or in the seated position. Personally, I think it’s hard to stabilize while standing and unless you’ve got a resting HR in the 40s, laying or seated will be the best.
Great article! Any chance of posting a bibliography for the additional research cited?
Here you go, Vin. It’s in the order the article mentioned them –
Selman A, MacDonald A, Kitney R, te al. The interaction between heart rate and respiration. Part I: experimental studies in man. Automedica 1982; 4: 131-9
Eckberg DL. Sympathovagal balance: a critical appraisal. Circulation 1997; 96(9): 3224-32
Gudemez E, Ozer K, Cunningham B, Siemionow K, Browne D, and Siemionow M.
Dehydroepiandrosterone as an enhancer of functional recovery following crush injury to rat sciatic nerve. Microsurgery 2002; 22: 234-241
Lee W, Chen S, Wu M, Hou C, Lai Y, Laio Y, Lin C, and Kuo C. The role of deydroepiandrosterone levels on physiologic acclimatization to chronic mountaineering activity. High Alt Med Biol 2006; 7:228-236
Uusitalo A.L., A.J. Uusitalo, and H.K. Rusko. Endurance training, overtraining and baroreflex sensitivity in female athletes. Clin Physiol 1998; 18: 510-520
Uusitalo A.L., A.J. Uusitalo, and H.K. Rusko. Exhaustive endurance training for 6-9 weeks did not induce changes in intrinsic heart rate and cardiac autonomic modulation in female athletes. Int J Sports Med 1998; 19: 532-540
Hohnloser S.H., Klingenheben T., Zabel M., Schroder F., and Just H. Intraindividual reproducibility of heart rate variability. Pace 1992; 15:2211-2214.
Huikuri H.V., Kessler K.M., Terracall E., Castellanos A., Linnaluoto M.K., and Myerburg R.J. Reproducibility and circadian rhythm of heart rate variability in healthy subjects. Am J Cardiol 1990; 65: 391-393
Allgorve JE, Gomes E, Hough J, Gleeson M. Effects of exercise intensity on salivary antimicrobial proteins and markers of stress in active men. J Sports Sci 2008; 26(6): 653-61
-Eric
great summary – only one inaccuracy: Allgorve et al. measured the concentration of salivary immunoglobulin A in saliva produced by cells in the salivary gland. s-IgA is a protein produced in saliva by salivary cells and contributes to the defense of mucous membranes from pathogens.